Post 2: The Range of SPP Services
By: Sarah Castillo, PhD, CMPC, UWS sport and performance psychology program director
In the first post in this series, we talked about the “continuum of mental health.” As you recall, mental health is not simply the absence of mental illness – it’s more nuanced than that. Performers exist at every point along the continuum from “in crisis” to “excelling,” and that means there must be appropriately trained sport and performance psychology (SPP) practitioners available to work with them. Of course, the types of services provided depend upon the needs of the client and the expertise of the SPP practitioner. In general, these services can be placed into one of two categories: clinical or performance. We’ll talk about the differences between the two, but first, it’s essential to talk about the underlying requirements of both.
If you’ve decided to work in a mental health career, whether you’re interested in doing clinical or performance work, you’ve got to be proficient at demonstrating basic counseling skills. These skills include, but are not limited to, the ability to 1) demonstrate empathy and listening skills; 2) the ability to paraphrase, challenge, and question; 3) the competency to read and respond to both verbal and nonverbal cues; and 4) the ability to collaborate effectively with the client from initial assessment to termination of the helping relationship. Often, people enter the helping professions thinking “I’m the one all of my friends come to when they need advice,” or “all of my friends tell me how easy I am to talk to.” While that’s flattering, and likely says something about an innate ability to help, it’s essential to know that “helping” is not the same as “advice-giving,” and being “easy to talk to” is different than serving as a guide toward lasting behavioral change. Basic counseling skills are common to both clinical and performance work with performers, but they are by no means easy to learn and develop.
Now that we’ve talked about the common skills and abilities that SPP practitioners across the continuum of mental health must have, lets dive deeper into the two general types of services. For reference, below is a linear depiction of the Delphis (2020) proposed continuum of mental health.
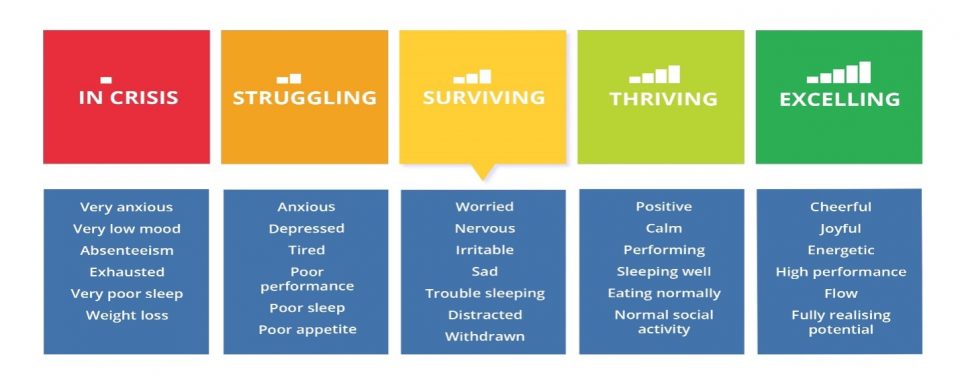
In order to provide clinical services, SPP practitioners must hold a state-issued license as a clinical mental health provider. When working with performers experiencing mental health distress (i.e., “in crisis” or “struggling”), services include the diagnosis and treatment of mental illness according to the classifications in Diagnostic and Statistical Manual (DSM). The goal of clinical services is “restorative.” That is, treatment focuses on helping the performer to regain positive control over thoughts, emotions, and behaviors. Examples of these state-licensed professions include psychologists, clinical social workers, marriage and family therapists, and clinical mental heal counselors. In every case, clinical practitioners are held to the standards and particular ethical codes of their profession, including the requirement to refer clients out when their needs do not match the role and/or expertise of the SPP practitioner.
SPP practitioners providing performance services work with performers and groups who are already “thriving” or “excelling.” Observations, interviews and assessments are conducted to determine the performer’s needs. Next, mental skills interventions are designed and implemented to improve performance beyond the current level. Along the way, the practitioners and performers work together to assess effectiveness and make changes when and where necessary. Currently, the only accredited competency standard in sport and performance consulting is the Certified Mental Performance Consultant (CMPC®) credential offered through the Association of Applied Sport Psychology (AASP). Similar to clinical services, the provision of performance services requires adherence to the standards and particular ethical codes of the profession, including the requirement to refer clients out when their needs do not match the role and/or expertise of the SPP practitioner.
But who works with performers who are “surviving”? If you’ve been paying attention, you’ve noticed that there’s still one category in the mental health continuum that hasn’t been addressed. Those performers who may be classified as “surviving” might be best served by either clinical services, performance services, or both. This makes it essential for SPP practitioners to pay close attention to performers’ thoughts, emotions and behaviors. While the presenting issue may be performance-related, clinical issues may arise. Conversely, the presenting issue might best be addressed by a clinical practitioner, but during the course of treatment performance-related issues might appear. In either case, the SPP practitioner must have the training and expertise to recognize the additional impact of clinical or performance issues and make the appropriate referral.
At UWS, we believe that the “dual relationships” clause present in both clinical mental health and mental performance consulting ethical codes expressly prohibits SPP practitioners from working with a single performer on both clinical and performance issues. That is, even when an SPP practitioner is dually trained (i.e., both a licensed clinician and a CMPC®), they may not fulfill both roles with the same client. Although from the practitioner’s perspective it may seem easy to “switch hats” based upon the issue the performer brings to session, the prohibition is developed with the client’s perspective in mind; that is, is the client aware of when the “hats” have been switched? Does the client know which hat the SPP practitioner is wearing when they visit a training session? Because, at any point, the client may be negatively impacted by the confusion or anxiety these dual roles cause, it is unethical.
Check out the third installment of the “What is Sport and Performance Psychology?” series that covers how the UWS SPP and CMHC programs prepare students to build their careers in these growing professions.
